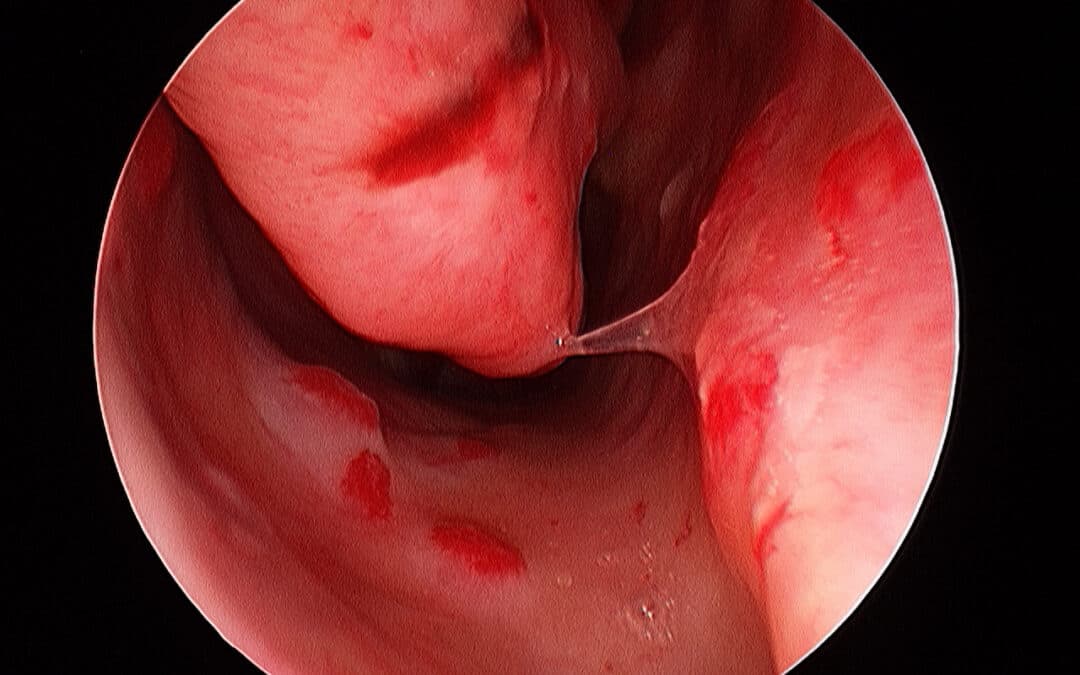
HHT Nosebleeds Treatment in Australia: A Specialist ENT Algorithm for Refractory Epistaxis
Hereditary hemorrhagic telangiectasia (HHT) is a genetic vascular disorder characterised by fragile, abnormal blood vessels. The most common and often most disabling manifestation is recurrent epistaxis. For many patients in Australia, HHT-related nosebleeds progress from occasional inconvenience to chronic haemorrhagic disease requiring iron infusions, transfusions, repeated procedures and multidisciplinary care.
This article outlines an evidence-based treatment framework for HHT nosebleeds and presents a practical, phenotype-driven escalation strategy for patients who fail lubricants, tranexamic acid and ablation therapy. Its my professional modification of the Consensus statement with the evidence basis for what surgical procedures and when.
Why Are Nosebleeds So Common in HHT?
HHT is caused by mutations affecting angiogenesis pathways, most commonly involving ENG or ACVRL1 genes. The result is abnormal vascular development. Within the nasal cavity this leads to superficial telangiectasias with thin walls and reduced structural support, predisposing to recurrent bleeding with airflow, dryness and minor trauma.
Stepwise Management of HHT Epistaxis
The Second International HHT Guidelines provide a structured management framework [1]. However, once initial therapy fails, escalation should reflect bleeding phenotype rather than follow a purely linear pathway.
Step 1: Moisturising Therapy
Daily saline sprays, gels and humidification form the foundation of management. Reducing crusting and mucosal trauma decreases bleeding frequency but does not alter angiogenic drive.
Step 2: Tranexamic Acid
Oral tranexamic acid stabilises clot formation and can reduce bleeding severity in patients with persistent epistaxis [1]. It does not modify telangiectasia formation but is useful adjunctive therapy.
Step 3: Ablative Therapies
KTP laser, radiofrequency ablation, coblation and sclerotherapy reduce bleeding by coagulating visible telangiectasias. While effective, benefits are often temporary, and repeated ablation may result in septal damage [1].
When Ablative therapy and TXA Fail: A Phenotype-Driven Strategy
Phenotype 1: Multi-System Bleeding
Patients with severe anaemia, transfusion dependence or concurrent gastrointestinal bleeding represent a systemic angiogenic phenotype. In this group, intravenous bevacizumab targets VEGF-mediated angiogenesis and has demonstrated reductions in Epistaxis Severity Score and improvements in haemoglobin levels [2].
Phenotype 2: Nasal-Dominant Refractory Disease
In patients with predominantly nasal bleeding and limited systemic involvement, septodermoplasty may provide durable benefit. This surgical technique replaces fragile septal mucosa with a split-thickness skin graft, reducing telangiectasia density and mechanical trauma [3].
Phenotype 3: Temporary Stabilisation
Silicone (Silastic) septal splints reduce airflow trauma and may provide temporary control or serve as bridging therapy in selected patients [4].
Salvage Therapy: Nasal Closure
Nasal closure (Young’s procedure) eliminates airflow through the nose and remains the definitive salvage option for life-threatening or transfusion-dependent epistaxis after failure of other interventions [1,5].
Practical Specialist Algorithm
Step 1: Moisturisation and iron optimisation
Step 2: Tranexamic acid
Step 3: Coblation, Laser or ablative therapy
Step 4: Stratify phenotype
• Multi-system bleeding → Intravenous bevacizumab
• Nasal-dominant disease → Septodermoplasty
• Temporary control required → Silicone splints
• Catastrophic refractory disease → Nasal closure
Escalation should reflect disease biology rather than simply symptom severity.
Frequently Asked Questions About HHT Nosebleeds
Can HHT nosebleeds be cured?
Hereditary hemorrhagic telangiectasia (HHT) is a genetic condition and cannot be cured. However, the frequency and severity of nosebleeds can often be substantially reduced. Management includes regular nasal moisturising therapy, tranexamic acid, targeted ablative procedures such as laser treatment, and escalation to systemic or surgical options in refractory cases.
When should tranexamic acid be used for HHT epistaxis?
Tranexamic acid is typically considered when regular moisturising therapy alone does not provide adequate control. It works by stabilising clot formation and may reduce bleeding severity. It is usually used in conjunction with local ENT measures rather than as a standalone treatment.
What is the role of laser/Coblation therapy in HHT nosebleeds?
Laser and other ablative therapies treat visible telangiectasias within the nasal cavity. These procedures can reduce bleeding frequency and improve quality of life. However, because HHT is driven by ongoing angiogenesis, new telangiectasias may form over time, and repeat treatments or escalation may be necessary.
When is bevacizumab considered for HHT-related nosebleeds in Australia?
Intravenous bevacizumab may be considered in severe or refractory cases, particularly in patients with multi-system bleeding, recurrent iron infusions, or transfusion dependence. Bevacizumab targets vascular endothelial growth factor (VEGF) and addresses the underlying angiogenic drive of the disease. Suitability and access require specialist assessment.
What is septodermoplasty and who is it for?
Septodermoplasty is a surgical procedure in which fragile septal mucosa is replaced with a split-thickness skin graft. It is generally considered in patients with nasal-dominant, refractory HHT epistaxis who have not achieved adequate control with medical therapy and laser treatment.
When is nasal closure (Young’s procedure) used?
Nasal closure is a salvage procedure reserved for severe, refractory epistaxis, particularly when bleeding is life-threatening or transfusion-dependent and other treatments have failed. The procedure permanently stops nasal airflow and requires careful counselling before proceeding.
References
- Faughnan ME, Mager JJ, Hetts SW, Palda VA, Lang-Robertson K, Buscarini E, et al. Second International Guidelines for the Diagnosis and Management of Hereditary Hemorrhagic Telangiectasia. Ann Intern Med. 2020;173(12):989-1001.
- Li W, Bai J, Symons A, Banting J, Rimmer J. The Effect of Systemic Bevacizumab on Epistaxis-Related Outcomes in Hereditary Hemorrhagic Telangiectasia: A Systematic Review and Meta-Analysis. Int Forum Allergy Rhinol. 2025;15(8):803-817.
- Harvey RJ, Kanagalingam J, Lund VJ. The impact of septodermoplasty and potassium-titanyl-phosphate laser therapy in the treatment of hereditary hemorrhagic telangiectasia-related epistaxis. Am J Rhinol. 2008;22(2):182-187.
- Matti E, Maiorano E, Nacu B, Luceri A, Sovardi F, Siragusa V, et al. Silicone septal splint for recurrent epistaxis in HHT patients: experience of a national referral centre. Acta Otorhinolaryngol Ital. 2023;43(Suppl 1):S28-S33.
- Bickerton R, Gera R, Ross T, Rennie C. Is nasal closure an effective treatment for severe refractory epistaxis in HHT? Rhinology. 2025;63(2):153-162.Whitehead KJ, Sautter NB, McWilliams JP, et al. Effect of topical intranasal therapy on epistaxis frequency in patients with hereditary hemorrhagic telangiectasia: a randomized clinical trial. JAMA. 2016;316(9):943-951.
- Gaillard S, Dupuis-Girod S, Boutitie F, et al; ATERO Study Group. Tranexamic acid for epistaxis in hereditary hemorrhagic telangiectasia patients: a European cross-over controlled trial in a rare disease. J Thromb Haemost. 2014;12(9):1494-1502.
- Geisthoff UW, Seyfert UT, Kübler M, et al. Treatment of epistaxis in hereditary hemorrhagic telangiectasia with tranexamic acid—a double-blind placebo-controlled cross-over phase IIIB study. Thromb Res. 2014;134(3):565-571.
- Benaim EH, Kallenberger EM, Mirmozaffari Y, Klatt-Cromwell C, Ebert CS Jr, Kimple AJ, et al. Surgical Management of Moderate to Severe Epistaxis in Hereditary Hemorrhagic Telangiectasia: Systematic Review and Meta-Analysis. Am J Rhinol Allergy. 2025;39(2):159-168.
- Thiele B, Abdel-Aty Y, Marks L, Lal D, Marino M. Sclerotherapy for Hereditary Hemorrhagic Telangiectasia-Related Epistaxis: A Systematic Review. Ann Otol Rhinol Laryngol. 2023;132(1):82-90.