Why “Blocked Nose” Doesn’t Always Mean Blocked Airflow
The importance of objective testing in nasal breathing
Many patients come to clinic saying they have a “blocked nose” or “nasal congestion.” It is one of the most common symptoms in ENT practice. Yet what patients describe as congestion can mean very different things medically.
Some patients truly have restricted airflow through the nose, while others have a sensation of stuffiness caused by inflammation, mucus, or nerve signalling in the nasal lining. These two problems feel similar, but they are not the same — and they require very different treatments.
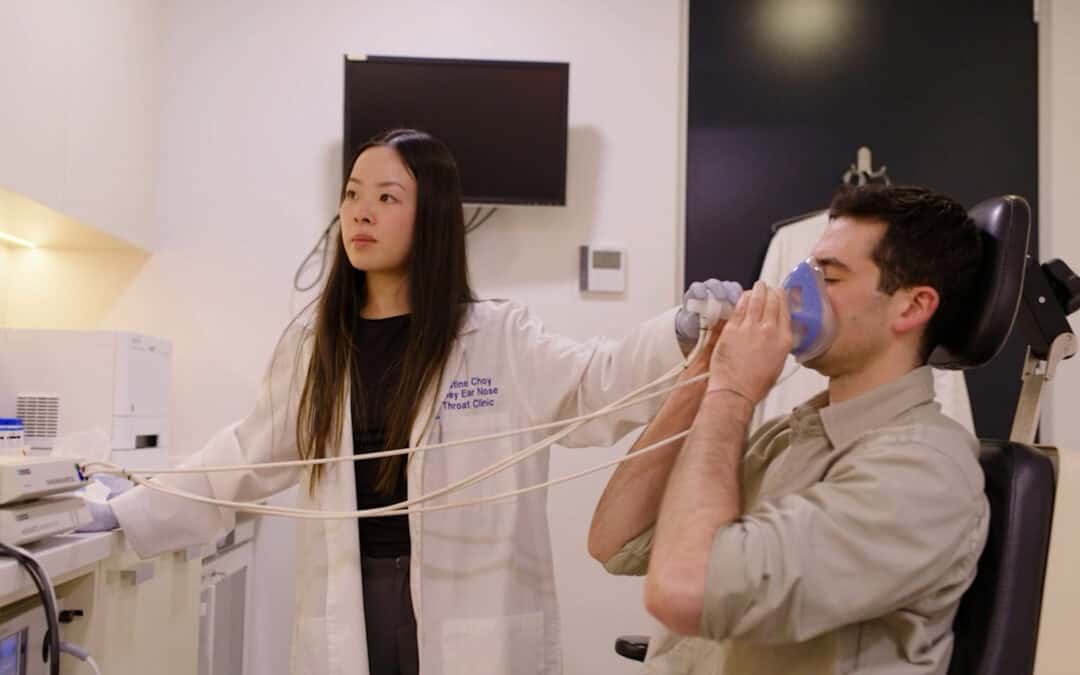
At the Sydney ENT Clinic NoseLab, we use specialised testing to determine whether a patient’s symptoms are caused by real airflow obstruction or by other nasal conditions. This distinction is critical before recommending treatments such as medication, allergy therapy, or surgery.
You can learn more about the facility here:
https://richardharvey.sydneyentclinic.com/services/nose-lab/
Nasal congestion vs nasal obstruction: not the same thing
Patients often use the word “congestion” to describe several different sensations:
-
difficulty breathing through the nose
-
pressure in the face or sinuses
-
a “stuffy” or heavy feeling
-
mucus in the nose or throat
However, these symptoms do not always reflect a physical blockage of airflow.
Research comparing patient and doctor interpretations of “nasal congestion” shows that patients often associate it with pressure, mucus, or headaches, whereas clinicians define congestion primarily as reduced airflow through the nose.
Understanding this difference is essential because treatments aimed at improving airflow (such as septoplasty or nasal valve surgery) may not help symptoms caused by inflammation or nerve signalling.
How the nose senses airflow
The sensation of nasal breathing is not produced by airflow sensors. Instead, it is generated by cooling of the nasal lining as air passes through it.
Cold-sensitive receptors in the trigeminal nerve (TRPM8 receptors) detect this cooling effect and signal to the brain that airflow is present.
Medicine today outline_RJH_edit…
This explains several common experiences:
-
Menthol or eucalyptus inhalers can make the nose feel clearer without actually improving airflow.
-
Allergic inflammation or thick mucus can make the nose feel blocked even when airflow is normal.
-
Patients sometimes feel severe obstruction despite adequate nasal airway space.
In other words, perception and physiology do not always match.
Why objective testing matters
Because symptoms alone can be misleading, objective testing is increasingly important in nasal medicine.
At the NoseLab we combine:
-
detailed nasal endoscopy
-
functional airflow testing
-
physiological assessment of nasal resistance
These tools allow us to determine whether symptoms are caused by:
-
Structural obstruction
Examples include septal deviation, nasal valve narrowing, or turbinate enlargement. -
Inflammatory congestion
Often related to allergy, rhinitis, infection, or environmental irritants. -
Functional or sensory disorders
Where the perception of airflow does not correspond with measurable airflow.
Objective testing helps prevent unnecessary surgery and ensures the correct treatment is chosen.
Rhinomanometry: measuring nasal airflow
One of the most useful tools for evaluating nasal breathing is rhinomanometry.
This test measures:
-
airflow through each side of the nose
-
pressure changes during breathing
-
nasal airway resistance
By quantifying nasal resistance during normal breathing, rhinomanometry helps distinguish:
-
fixed anatomical obstruction
-
reversible congestion caused by inflammation
It is considered one of the most reliable objective tests for evaluating nasal airflow and monitoring treatment response.
For example:
-
If airflow improves significantly after a nasal decongestant, the problem is likely inflammatory (such as allergy).
-
If airflow remains restricted, a structural issue such as nasal valve narrowing may be present.
This information helps guide decisions about medical therapy, allergy treatment, or surgery.
What research tells us about nasal symptoms
Interestingly, research shows that symptoms do not always correlate strongly with objective airflow measurements.
Studies from our group and others have demonstrated that patients’ perception of nasal obstruction can be influenced by multiple factors, including mucosal inflammation and even emotional health.
This highlights an important point:
treating the structure of the nose alone does not always solve the problem.
Instead, effective management requires understanding the full physiological picture.
Using nasal endoscopy to identify inflammation
Nasal endoscopy provides a detailed view of the inside of the nose and sinuses.
Certain endoscopic findings can suggest allergy-driven inflammation, including:
-
middle turbinate oedema
-
watery secretions
-
inferior turbinate hypertrophy
These features have been shown to correlate with allergic airway disease in systematic reviews of nasal endoscopy findings.
Our research group has contributed extensively to understanding these patterns of disease.
You can see an example of nasal examination techniques here: Endoscopic features of inhalant allergy
And examples explaining nasal obstruction and congestion: 2024-Harvey et al Cheif complaint nasal congestion
The role of the NoseLab
The NoseLab at Sydney ENT Clinic is designed to provide comprehensive evaluation of nasal breathing using advanced diagnostic tools.
Testing may include:
-
rhinomanometry
-
nasal endoscopy
-
airflow resistance testing
-
assessment before and after decongestants
-
evaluation of nasal valve function
This approach allows us to move beyond simple visual examination and measure how the nose actually functions during breathing.
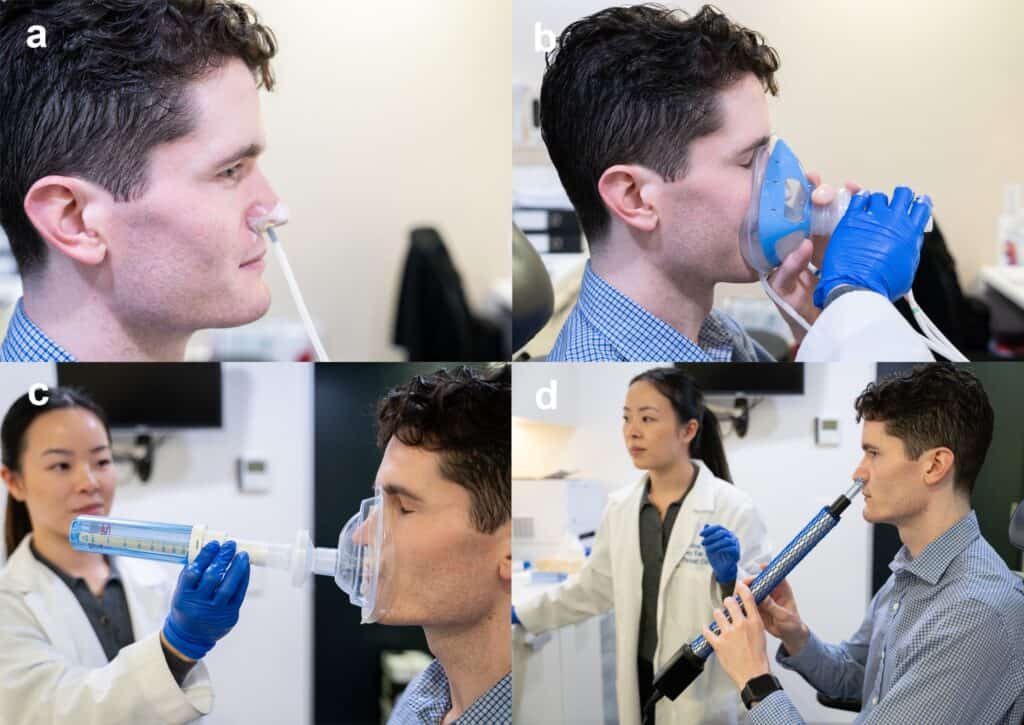
Rhinomanometry is the most reliable testing and measures true airflow (a & b). Nasal peak inspiratory flow (c) measures collapsibility and the shape or cross-sectiona is measured by acoustic rhinomanometry (d)
The goal is to provide patients with:
-
accurate diagnosis
-
personalised treatment plans
-
avoidance of unnecessary procedures
When should you consider objective testing?
Objective nasal airflow testing can be helpful if you experience:
-
persistent nasal blockage despite treatment
-
poor sleep related to nasal breathing
-
ongoing symptoms after nasal surgery
-
uncertainty about whether surgery may help
-
complex symptoms where scans appear normal
Understanding whether symptoms reflect true airflow obstruction or inflammatory congestion is the first step toward effective treatment.
Many patients are unsure whether their nasal congestion is caused by true airflow obstruction or by inflammation within the nose. The following questions address common concerns about nasal breathing and objective airflow testing.
Frequently Asked Questions About Nasal Congestion and Nasal Airflow Testing
What is the difference between nasal congestion and nasal obstruction?
Nasal congestion and nasal obstruction are often used interchangeably, but they are not the same. Nasal obstruction refers to a physical restriction of airflow through the nose, usually caused by structural problems such as a deviated septum or nasal valve narrowing. Nasal congestion, however, often refers to the sensation of a blocked or stuffy nose caused by inflammation, mucus, or swelling of the nasal lining. Many patients feel congested even when airflow through the nose is normal.
How can doctors measure whether my nose is actually blocked?
Doctors can objectively measure nasal airflow using specialised tests such as rhinomanometry. This test measures the pressure and airflow through each side of the nose during normal breathing. By calculating nasal airway resistance, rhinomanometry helps determine whether symptoms are caused by a true airflow obstruction or by inflammatory congestion from conditions such as allergy or rhinitis.
What is rhinomanometry?
Rhinomanometry is a diagnostic test used to measure nasal airflow and nasal resistance during breathing. It works by measuring the pressure difference between the front and back of the nose while airflow is recorded. The results show whether the nasal airway is physically restricted and whether the obstruction improves after using a nasal decongestant.
Why do some people feel blocked even when their nose is open?
The sensation of nasal breathing depends largely on cooling of the nasal lining as air flows through it. Nerve receptors in the nose detect this cooling effect and signal the brain that airflow is present. When inflammation, mucus, or swelling interfere with this cooling sensation, patients may feel congested even if airflow is normal.
Can allergy cause nasal congestion without blocking airflow?
Yes. Allergic rhinitis and other inflammatory conditions can cause swelling of the nasal lining, increased mucus production, and nerve irritation. These changes can create a strong sensation of congestion even when the airway remains relatively open.
When should someone consider objective nasal airflow testing?
Objective testing may be helpful if you experience:
-
persistent nasal blockage despite treatment
-
difficulty breathing through the nose during sleep
-
ongoing symptoms after previous nasal surgery
-
uncertainty about whether surgery may improve breathing
-
symptoms of nasal congestion despite normal scans or examinations
Testing helps determine whether symptoms are due to structural obstruction or inflammatory congestion.
Can nasal airflow testing help decide if surgery is necessary?
Yes. Objective airflow testing can help determine whether surgery is likely to improve breathing. If testing shows that airflow obstruction is caused by structural narrowing, procedures such as septoplasty or nasal valve surgery may help. If airflow is normal, treatment may instead focus on allergy control or medical therapy.
What tests are performed in a specialised nasal airflow laboratory?
In a specialised nasal function clinic such as the NoseLab, testing may include:
-
rhinomanometry to measure airflow resistance
-
nasal endoscopy to visualise internal structures
-
nasal airflow measurements before and after decongestants
-
evaluation of nasal valve function
-
assessment of inflammatory conditions such as allergy or rhinitis
These tests help provide a comprehensive evaluation of nasal breathing.
Why is my nose always blocked at night?
Many people notice that their nose feels more blocked when lying down at night. This occurs because body position changes blood flow to the nasal lining. When you lie down, increased venous pressure causes the turbinates (structures inside the nose) to swell slightly. This is part of the normal nasal cycle, where one side of the nose becomes more congested while the other opens. In people with allergy, inflammation, or structural narrowing, this normal cycle can become exaggerated and produce significant nighttime congestion.
Can a deviated septum cause nasal congestion?
Yes. A deviated septum, where the cartilage or bone dividing the nasal passages is off-centre, can narrow one or both sides of the nasal airway and reduce airflow. However, many people with septal deviation breathe normally and do not experience symptoms. Nasal congestion is often caused by inflammation from allergy or rhinitis rather than septal anatomy alone. Objective airflow testing can help determine whether a septal deviation is actually responsible for breathing problems.
Why does menthol make my nose feel clearer?
Menthol and similar substances stimulate cold-sensitive nerve receptors in the nasal lining. These receptors signal to the brain that air is moving through the nose, creating a sensation of improved airflow. However, menthol usually does not change the physical size of the nasal airway or improve airflow resistance. It simply alters the perception of breathing, which is why products containing menthol, eucalyptus, or similar compounds can make the nose feel clearer without treating the underlying cause of congestion.
Learn more
If you would like to learn more about advanced nasal testing and evaluation, visit:
NoseLab:
https://richardharvey.sydneyentclinic.com/services/nose-lab/
Research publication:
https://pubmed.ncbi.nlm.nih.gov/35726828/