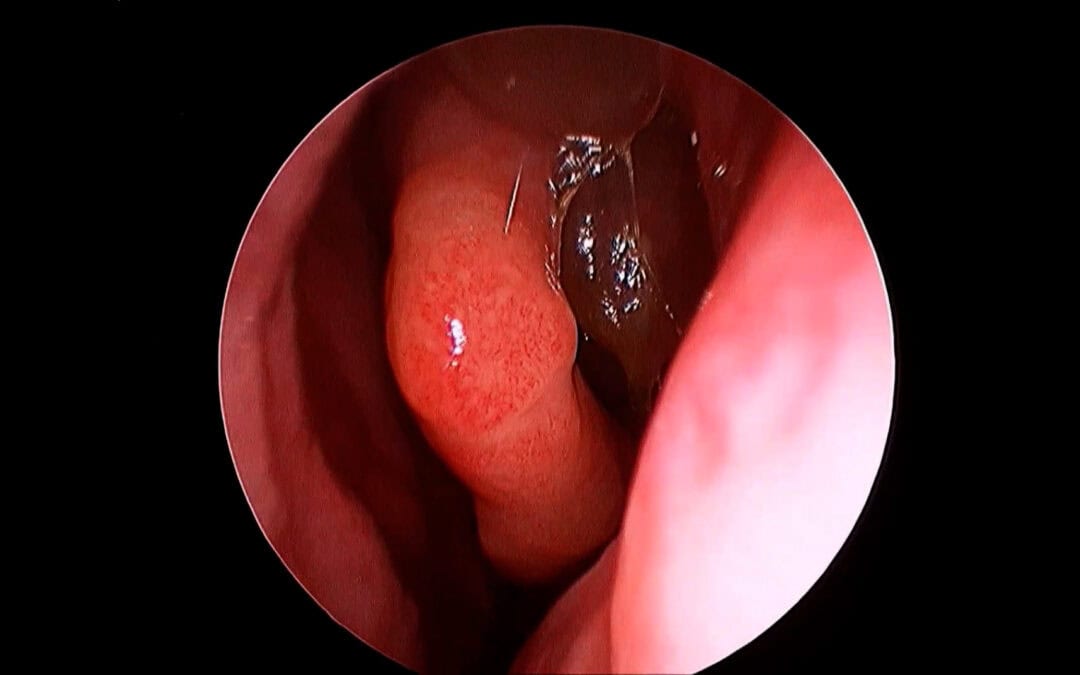
The management of chronic rhinosinusitis (CRS)—particularly diffuse type-2 disease such as CRSwNP or eosinophilic CRS—has entered a new era.
Biologic therapies have transformed outcomes. But an important question remains:
Can biologics replace surgery—or is the combination the optimal approach?
In a recent presentation at the ASOHNS ASM in Hobart, I explored the evolving role of surgery in the biologic era and why combining surgery and biologics in CRS is often essential to achieving remission.
The Traditional Pathway—and Its Limitations
Patients with diffuse CRS typically follow a familiar pathway:
- topical corticosteroids
- short courses of oral steroids
- endoscopic sinus surgery
- revision surgery in refractory cases
Biologics such as dupilumab, mepolizumab, and tezepilumab now offer a powerful new option.
This has led to a natural question:
Why not just use biologics and avoid surgery altogether?
The answer is more nuanced.
Surgery Still Matters in the Biologic Era
Randomised trials of biologics show clear efficacy, but they also reveal an important signal:
👉 Patients with prior surgery behave differently
Post-hoc analyses from both mepolizumab and dupilumab trials suggest that:
- prior surgery is often a marker of more severe disease
- but also of greater responsiveness to biologics
This may reflect:
- reduced tissue remodelling
- improved drug access
- altered inflammatory burden
But beyond this, we must consider what surgery actually achieves.
Surgery Is Not Just About Access
It is often said that surgery improves topical drug delivery.
That is true—but incomplete.
Surgery also:
- removes inflammatory tissue
- reduces polyp burden
- improves mucociliary clearance
- addresses mechanical obstruction
- removes co-pathologies such as REAH or mucus plugging
These are not trivial effects.
They fundamentally alter the disease environment.
The Importance of Surgical Completeness
One of the most important concepts emerging from recent work is extent of surgery.
Studies using the ACCESS score and similar metrics show that:
👉 More complete surgery is associated with better outcomes in biologic-treated patients
- Lower ACCESS scores (i.e. more complete surgery) → better symptom outcomes
- Greater surgical completeness predicts response to dupilumab
- In multivariate analysis, extent of surgery may be the dominant predictor of outcome
This aligns with our own work:
Extent of sinus surgery is associated with disease control in biologic-treated CRS
In this cohort:
- ~49% achieved remission/control overall
- Remission rates were dramatically higher with extended surgery:
- Draf III: ~61%
- Draf IIc: ~68%
- Draf IIa: ~9%
- Draf I: 0%
👉 Extent of surgery, not comorbdiites like AERD/Asthma, once on biologics, was the key determinant of outcome
Timing Matters: Surgery vs Biologics—or Both?
Another key question is sequencing:
- biologic first?
- surgery first?
- or combination?
Emerging evidence suggests:
👉 Combination therapy outperforms biologics alone
Randomised and real-world studies show:
- improved outcomes when biologics are combined with surgery
- greater symptom control
- reduced steroid dependence
Importantly, patients with incomplete prior surgery appear to benefit significantly from revision procedures—even when already on biologics. This work from Prof Palmer and UPenn on COSI supports this statement.
This reinforces a critical point:
Biologics do not correct structural disease. Surgery does.
The Goal Has Changed: Remission
Historically, we aimed to “improve symptoms.”
That is no longer enough.
The goal in 2026 is:
- no systemic steroids
- stable endoscopic findings
- low symptom burden
- durable disease control
👉 Remission
Achieving this requires addressing both:
- the inflammatory pathway (biologics)
- the structural and mechanical disease (surgery)
Avoiding Reductionist Thinking
One of the risks in the biologic era is reductionism:
viewing CRS as purely an inflammatory disease treatable with drugs alone
But diffuse CRS is more complex.
It includes:
- tissue remodelling
- polyp formation
- mucus stasis
- structural dysfunction
- coexisting pathologies
No single therapy addresses all of these.
The Future: Combination Therapy
The message from current evidence is clear:
- Surgeons need biologics
- Patients need surgery
- Outcomes are best when both are used appropriately
👉 Combination therapy offers the highest likelihood of remission
As we move forward, the question is no longer:
Surgery or biologics?
But rather:
How do we combine them optimally for each patient?
📺 Watch the full presentation here:
https://youtu.be/4dW-ZwKegW4
FAQ Section
Can biologics replace sinus surgery in CRS?
No. Biologics treat inflammation but do not address structural disease, tissue remodelling, or mucus obstruction.
Does surgery improve biologic response?
Yes. More complete surgery is associated with better outcomes and higher remission rates in biologic-treated CRS.
What is the goal of treatment in CRS today?
The goal is remission—no steroids, stable disease, and long-term control.
When should surgery be combined with biologics?
Combination therapy is most effective in diffuse type-2 CRS, especially when prior surgery is incomplete.