“Septal deviation and big turbinates” is not a diagnosis: why nasal obstruction often returns after surgery
One of the commonest referral patterns I see as a tertiary rhinologist is the patient who has had nasal surgery, initially felt better, and then slowly developed the same sense of nasal blockage again. These patients often arrive disappointed, sometimes angry, and usually confused. They have been told they had a “septal deviation and big turbinates”, underwent septoplasty, turbinate reduction or both, and expected a durable solution.
The problem is that “septal deviation and enlarged turbinates” is not a diagnosis. It is a description of anatomy.
That distinction matters. A diagnosis should explain why the nose feels blocked, why the problem developed, why it behaves the way it does, and why a particular treatment should work. A deviated septum may explain unilateral nasal obstruction, particularly if it follows trauma or has been present since adolescence. But it is a weaker explanation for progressive, bilateral nasal congestion that has developed over time without injury.
When the obstruction is generalised, alternates from side to side, worsens when lying flat, or is clearly affected by irritants, seasons or indoor environments, the cause is usually more than fixed anatomy. It is often rhinitis. The next question should be: what type of rhinitis, and what is driving it?
Congestion and obstruction are not always the same thing
Patients and clinicians often use the same words differently. Patients may use “congestion” to mean blocked airflow, pressure in the face, mucus in the throat, heaviness in the head or even headache. In contrast, rhinologists usually reserve “obstruction” for impaired nasal airflow and “congestion” for mucosal swelling or vascular engorgement.
This mismatch has been formally described. In a study of how patients and clinicians define “nasal congestion”, patients were much more likely than clinicians to include pressure-related symptoms, mucus-related symptoms and other non-obstructive symptoms in their definition of congestion.[1] This is why a patient can have a scan report mentioning a deviated septum or turbinate hypertrophy and still not have a useful diagnosis. The finding may be real, but it may not be the dominant cause of the symptom.
This issue is also central to our forthcoming Medicine Today feature article, How we breathe: Nasal congestion and treatment strategies, selected as the May feature article. The article emphasises that nasal congestion is more than a blocked nose: patient perceptions of pressure, mucus and airflow often diverge from clinical definitions, complicating diagnosis and management.
A practical distinction is this: a fixed anatomical obstruction tends to be consistent, often affecting one side more than the other, and may relate to trauma, nasal development, prior rhinoplasty or valve collapse. A physiological or inflammatory obstruction tends to vary. It may cycle from side to side, worsen when lying down, respond temporarily to decongestant spray, fluctuate with allergen exposure, or worsen in certain environments.
The second pattern is commonly turbinate-based and vascular, but the driver is often inflammatory, allergic, neurogenic or irritant-related rather than simply “large turbinates”.
The nose is not just a pipe
A simple but misleading model is that nasal breathing improves if the surgeon makes a larger tunnel. That is only partly true.
Humans do not directly “measure” airflow through mechanical airflow receptors in the nose. The sensation of clear nasal breathing is strongly influenced by cooling of the nasal lining as air passes across the mucosa. Trigeminal cold receptors, including TRPM8 receptors, help generate the perception of nasal patency.[2,3] This explains why menthol, eucalyptus or similar products can make the nose feel clearer without objectively increasing airflow.
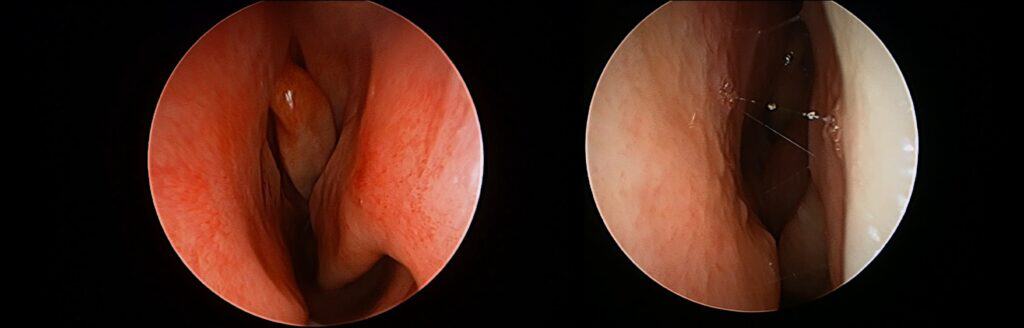
The nose on the left is not affected by allergy and has normal mucosa. The patient on the right has normal airflow but feels congested due the rhinitis reaction.
It also explains why surgery that creates space but does not restore healthy airflow over responsive mucosa may not solve the patient’s perceived congestion. Inflamed mucosa, thick mucus, vascular engorgement and tissue remodelling can all reduce the cooling signal. The patient may feel blocked even when the airway is not severely narrowed.
Conversely, after turbinate surgery, the early mechanical improvement may be obvious. But if the allergic or inflammatory drive persists, mucosal swelling and tissue remodelling can return.
The common mistake: treating the consequence, not the disease
Inferior turbinate hypertrophy is often the visible consequence of a long-standing mucosal disease. In allergic rhinitis, repeated allergen exposure can produce chronic inflammation, venous engorgement, glandular change and tissue remodelling. The turbinate becomes the visible structure that attracts surgical attention, but the allergy is the engine that keeps driving the process.
This is especially relevant in patients who do not present with classic “hay fever”. Many allergic patients do not volunteer itch, sneeze, watery rhinorrhoea or conjunctivitis. Their dominant symptom is obstruction. They may not intuitively think of allergy, and if the clinician does not test or examine for it, the disease is missed.
A more accurate formulation for many of these patients is not “septal deviation and big turbinates”. It is closer to:
Persistent rhinitis, often allergic or locally allergic, with turbinate and septal swell body tissue remodelling producing dynamic bilateral nasal obstruction.
That diagnosis leads to a different treatment plan…….not just surgery.
A negative allergy test does not always exclude allergy in the nose
Skin-prick testing and serum-specific IgE testing are important, but they are not perfect reflections of what is happening in the nasal mucosa. Some patients have negative skin and blood allergy tests but still react to allergen challenge directly in the nose. This is known as local allergic rhinitis.

Although epicutaneous tests for allergy are the gold standard, many patients with clear allergic rhinitis will have negative skin and serum tests. This doesnt mean that they dont have allergy, its just not present in surrogate markers for allergy in the nose. It can be as high 30%.
The concept is often referred to as “entopy” — allergy localised to the target organ rather than detectable systemically. A useful Australian shout-out belongs to Professor Simon Carney, whose work helped establish the idea that patients could show evidence of allergy in the absence of conventional systemic atopy.[4] The term “entopy” was later used in the local allergy paradigm literature to describe this nose-localised allergic response.[5]
This matters clinically. If a patient has a strongly allergic history — for example, seasonal symptoms, indoor dust mite pattern, morning congestion, turbinate oedema or mucus changes on endoscopy — a negative skin or serum test should not automatically close the door on allergy.
Hamizan and colleagues systematically reviewed nasal allergen provocation testing in allergic and non-allergic rhinitis. Across 46 studies, nasal allergen reactivity was present in 86.3% of patients classified as allergic rhinitis by systemic testing, but also in 24.7% of patients classified as non-allergic rhinitis.[6] The authors concluded that local allergen reactivity is demonstrated in about one quarter of patients previously considered non-allergic.
That finding is not academic hair-splitting. It changes how patients should be treated. A patient labelled “non-allergic” may still have an allergic reaction in the nose and may still be suitable for allergy-directed therapies.
Why turbinate surgery can feel good — then fade
Turbinate reduction can be very effective. It creates space, reduces vascular tissue volume, and can improve nasal airflow. The issue is not that turbinate surgery is poor surgery. The issue is that it is often being asked to do the wrong job.
Surgery can reduce the tissue burden. It does not, by itself, switch off the allergic or inflammatory process that enlarged the tissue in the first place.
The long-term data are important here. De Corso and colleagues prospectively followed 305 patients with rhinitis who underwent radiofrequency volumetric inferior turbinate reduction. Early results were favourable, with significant improvement in nasal stuffiness, nasal obstruction and mouth breathing.[7] But symptoms worsened after 36 months, with progressive recurrence, especially in allergic patients.
The relapse-free probability is the key figure. In the whole cohort, the cumulative probability of remaining relapse-free was 0.848 at 36 months but fell to 0.531 at 60 months. In allergic patients, it fell from 0.807 at 36 months to 0.357 at 60 months.[7] In plain terms, the benefit was real, but it diminished over time, and allergic rhinitis was associated with worse durability.
This does not mean turbinate surgery “failed”. It means the underlying biology kept operating.

The diminshing effects of a simple turbinate procedure over time (De Corso E, Bastanza G, Di Donfrancesco V, Guidi ML, Morelli Sbarra G, Passali GC, et al. Radiofrequency volumetric inferior turbinate reduction: long-term clinical results. Acta Otorhinolaryngol Ital. 2016;36(3):199-205.)
A later systematic review of surgical interventions for inferior turbinate hypertrophy also supports the general effectiveness of turbinate surgery, showing meaningful improvements in subjective nasal obstruction and objective airflow measures across multiple techniques.[8] But this should not be interpreted as a licence to label every bilateral blocked nose as a turbinate problem. The better conclusion is that turbinate surgery works best when the turbinate is genuinely the limiting structure and the disease process driving turbinate swelling has been identified.
This is the clinical pattern patients often describe: “It worked at first, then slowly stopped working.”
That slow loss of benefit should not automatically be interpreted as poor surgical technique. In many cases, the real problem is that the underlying rhinitis was never properly diagnosed, treated or modified.
Why intranasal steroid failure does not prove the problem is surgical
Another common heuristic is: try a nasal steroid spray; if it does not work, diagnose septal deviation and enlarged turbinates; then operate.
That is too simplistic.
A failed nasal spray trial does not prove that anatomy is the primary cause. It may mean the spray was poorly delivered, poorly adhered to, not strong enough, not the right treatment for the mechanism, or introduced too late to reverse established tissue remodelling. Or simply the initial benefit is not in align with patient expectations.
But patients with normal airflow on testing are the greatest risk from low benefit from septal and turbinate surgery in particular.
In persistent allergic rhinitis, especially house dust mite–driven disease, the relevant question is often not “did a spray help?” but “is this a chronic allergic airway disease requiring disease modification?”
Allergen immunotherapy is fundamentally different from symptom suppression. Antihistamines and intranasal corticosteroids may reduce symptoms while being used. Immunotherapy aims to reduce the immune response to the allergen itself. That is why, in selected patients, it should be considered earlier rather than after years of progressive tissue change.
This does not mean every patient needs immunotherapy. It means the diagnosis should be made properly before surgery is offered as the next step.
The pattern that should make clinicians pause
A simple septal deviation can explain unilateral obstruction. A single-sided blocked nose after trauma is a different problem from a patient who says:
“My nose blocks on both sides.”
“It changes sides.”
“It is worse lying flat.”
“It is worse overnight or in the morning.”
“It improves briefly with decongestant spray.”
“It has slowly developed over years.”
“I never had trauma.”
“I had turbinate surgery and it helped for a while, then wore off.”
That pattern should trigger a rhinitis workup, not just an anatomical label.
Assessment may include nasal endoscopy, allergy testing, objective airflow testing where available, decongestant response, and careful separation of airflow symptoms from pressure, mucus, sleep, fatigue and anxiety-related breathing concerns.
Rhinomanometry and nasal peak inspiratory flow can be useful because they test whether obstruction is truly airflow-related and whether it is reversible.[9] This matters before offering more surgery to a patient whose main symptom may not be mechanical obstruction.
Surgery still has a role — but it must be integrated
The correct conclusion is not “avoid turbinate surgery”. That would be just another simplistic rule.
Turbinate surgery can be valuable when tissue remodelling has become a major contributor to obstruction. In some patients, immunotherapy or pharmacotherapy improves the inflammatory component, but the remodeled turbinate or septal swell body remains too bulky. In those patients, surgery can restore airflow while disease-modifying therapy reduces the risk of the same process recurring.
This is also why the sequence of care matters. A patient who has substantial allergic inflammation and turbinate remodelling may need both disease modification and anatomical optimisation. Surgery may improve the airway, but immunotherapy or other medical strategies may be needed to prevent the same mucosal process from continuing.
The better model is integrated treatment:
First, define the symptom: airflow obstruction, congestion, pressure, mucus or mixed symptoms.
Second, identify the mechanism: fixed anatomy, allergic rhinitis, local allergic rhinitis, nasal hyperreactivity, irritant exposure, medication effect, rhinitis medicamentosa, chronic rhinosinusitis or a functional overlay (anxiety/hyperventilation/panic disorder/SSD).
Third, match treatment to mechanism: immunotherapy for relevant allergic drivers, pharmacotherapy for symptom control, irritant cessation where relevant, and surgery where anatomy or tissue remodelling is genuinely limiting airflow.
This is particularly important for patients who have already had “low-value” nasal surgery. Many are not wrong about their symptoms. They are wrong about the explanation they were given — or the explanation was incomplete.
The key message
“Septal deviation and enlarged turbinates” is a finding. “Congested nose” is a symptom. Neither is a proper diagnosis.
When patients have progressive bilateral nasal obstruction, alternating congestion, postural blockage or loss of surgical benefit over time, the clinician should look beyond anatomy. The question is not simply whether the septum is bent or the turbinates are large. The question is why the nasal airway is behaving that way.
In many patients, the answer is rhinitis — often allergic rhinitis or local allergic rhinitis — with turbinate-based vascular congestion and tissue remodelling. Surgery may still help, but only if it is used as part of a broader plan that addresses the disease process driving the obstruction.
Patients do better when treatment is directed at the cause, not the label.
References
- McCoul ED, Mohammed AE, Debbaneh PM, Carratola M, Patel AS. Differences in the intended meaning of congestion between patients and clinicians. JAMA Otolaryngol Head Neck Surg. 2019;145(7):634-640. doi:10.1001/jamaoto.2019.1073
- Harvey RJ, Roland LT, Schlosser RJ, Pfaar O. Chief complaint: nasal congestion. J Allergy Clin Immunol Pract. 2024;12(6):1462-1471. doi:10.1016/j.jaip.2024.04.028
- Sozansky J, Houser SM. The physiological mechanism for sensing nasal airflow: a literature review. Int Forum Allergy Rhinol. 2014;4(10):834-838. doi:10.1002/alr.21368
- Carney AS, Powe DG, Huskisson RS, Jones NS. Atypical nasal challenges in patients with idiopathic rhinitis: more evidence for the existence of allergy in the absence of atopy? Clin Exp Allergy. 2002;32(10):1436-1440. doi:10.1046/j.1365-2745.2002.01494.x
- Powe DG, Bonnin AJ, Jones NS. ‘Entopy’: local allergy paradigm. Clin Exp Allergy. 2010;40(7):987-997. doi:10.1111/j.1365-2222.2010.03536.x
- Hamizan AW, Rimmer J, Alvarado R, Sewell WA, Kalish L, Sacks R, Harvey RJ. Positive allergen reaction in allergic and nonallergic rhinitis: a systematic review. Int Forum Allergy Rhinol. 2017;7(9):868-877. doi:10.1002/alr.21988
- De Corso E, Bastanza G, Di Donfrancesco V, Guidi ML, Morelli Sbarra G, Passali GC, Poscia A, de Waure C, Paludetti G, Galli J. Radiofrequency volumetric inferior turbinate reduction: long-term clinical results. Acta Otorhinolaryngol Ital. 2016;36(3):199-205. doi:10.14639/0392-100X-964
- Zhang K, Pipaliya RM, Miglani A, Nguyen SA, Schlosser RJ. Systematic review of surgical interventions for inferior turbinate hypertrophy. Am J Rhinol Allergy. 2023;37(1):110-122. doi:10.1177/19458924221134555
- Chin D, Marcells G, Malek J, Pratt E, Sacks R, Harvey RJ. Nasal peak inspiratory flow as a diagnostic tool for differentiating decongestable from structural nasal obstruction. Rhinology. 2014;52(2):116-121. doi:10.4193/Rhino13.123
FAQ
Is a deviated septum always the cause of nasal obstruction?
No. A deviated septum can cause nasal obstruction, especially when symptoms are one-sided or followed nasal trauma. Progressive bilateral nasal congestion is often driven by rhinitis, allergy, turbinate swelling, nasal hyperreactivity or mucosal inflammation rather than septal anatomy alone.
Why did my turbinate surgery work at first and then stop working?
Turbinate surgery can reduce tissue volume and improve nasal airflow, but it does not always treat the inflammatory or allergic process that enlarged the turbinates. If rhinitis or allergy continues, turbinate swelling and nasal congestion can gradually return.
Can allergy cause nasal blockage without sneezing or itchy eyes?
Yes. Some patients with allergic rhinitis mainly experience nasal obstruction or congestion and do not have prominent sneezing, itching, watery discharge or eye symptoms. In these patients, allergy may be missed if clinicians only look for classic hay fever symptoms.
Can I still have nasal allergy if my skin-prick or blood allergy tests are negative?
Yes. Some patients have local allergic rhinitis, where the allergic reaction occurs in the nasal lining despite negative skin-prick or blood allergy tests. This has also been described as “entopy”.
When is turbinate surgery useful?
Turbinate surgery is useful when turbinate tissue remodelling or vascular congestion is a major contributor to nasal airflow limitation. It is most logically used as part of a broader plan that also addresses the underlying rhinitis, allergy or inflammatory driver.
What tests help distinguish congestion from fixed obstruction?
Nasal endoscopy, allergy testing, decongestant response, nasal peak inspiratory flow and rhinomanometry can help distinguish fixed anatomical obstruction from dynamic mucosal congestion.

